When 29-year-old entrepreneur Saima Thompson received a terminal diagnosis she began to understand the extent of the stigma some British South Asians attach to cancer. Here she explores the idea of “immigrant shame”, saying cultural taboos are fuelling health inequalities and costing lives.
When a swelling in my chest left me struggling to breathe in my sleep my GP suspected it might be a thyroid issue.
An ultrasound on my neck confirmed something wasn’t right and off to A&E I went for my life to be changed forever.
The medics baffled at the CT scan results. Could it be tuberculosis? Blood cancer? Not even the specialists could be clear. In fact the suspected swollen gland turned out to be a tumour which meant it was already too late. My cancer had metastasised (spread). I received a stage 4 lung cancer diagnosis at the age of 29.
My world changed colour, with a sudden rush of irrational and fearful emotions. I ran two restaurants at the time and was looking forward to my 30s, possibly beginning to see the fruits of my passionate labour.
 One in three lung cancer patients die within 90 days of diagnosis and GPs are not spotting the signs early due to lack of awareness and education. The result of this is poor advice and late staging of the cancer. Now statistically I have drawn the short straw, an exceptional circumstance as the average age of diagnosis is 85 to 89 years old. Yet the latest data tells us that lung cancer cases are on the rise in young women, the reason behind it yet to be clarified by the oncology world.
One in three lung cancer patients die within 90 days of diagnosis and GPs are not spotting the signs early due to lack of awareness and education. The result of this is poor advice and late staging of the cancer. Now statistically I have drawn the short straw, an exceptional circumstance as the average age of diagnosis is 85 to 89 years old. Yet the latest data tells us that lung cancer cases are on the rise in young women, the reason behind it yet to be clarified by the oncology world.
One question I have been asked relentlessly by friends, strangers, even health professionals that work in oncology… “Do you smoke?” as if I am at fault for having this illness on my head. It’s true that 72% of cases are smoking-related, so what about the 28% that aren’t?
I dabbled with cigarettes in my early 20s yet here I am with a terminal disease associated with old smokers.
There is a real stigma around lung cancer. It’s the third most common type of cancer in the UK (behind breast cancer and prostate cancer), yet it’s badly underfunded (termed a cancer “of unmet need”) and lacks both research and awareness due to its association with smoking.
The truth is you only need a pair of lungs to get cancer, and the same goes for any other body part and the other 200+ cancers that exist.
When I began to tell my family and friends, in my sick state, I started to come across cultural obstacles.
What those Macmillan booklets didn’t tell me to expect was the deafening silence from my South Asian family and wider community.
I waited three long weeks for biopsy results and got the news with my husband. I told my mother and she did not understand what I was saying. She did not understand cancer at all.
She replied: “You will get better.” I desperately tried to explain to her that what I have is incurable, but we may as well have been speaking different languages.
Read more: How can we stop mental health services failing young people?
I am a daughter to Pakistani immigrants, my mother came to the UK in 1987 and was a Punjabi homemaker, raising four girls, single-handedly after a marriage breakdown. She never worked or was given the opportunity to integrate properly.
She had visions of a better life with wishes to have further education but conservative values and Islamic traditions deprived her of that. This is not uncommon as only 38% of Pakistani and Bangladeshi women, aged 16 to 64, are employed in the UK – a shocking statistic when compared to the 73% of white British women who are currently in our workforce.
A lack of integration, conversation and education around basic health matters leaves a lot of the BAME population with great difficulties when it comes to flagging up or speaking about illness.
When telling extended family members I was met with comments such as “don’t worry we won’t tell anybody what you have” and “it’s all in God’s hands now”, “God will look after you.”
So this leads me to ask, why are we not talking? Why the silence? Why were family members making pacts to keep this health matter our dirty secret?
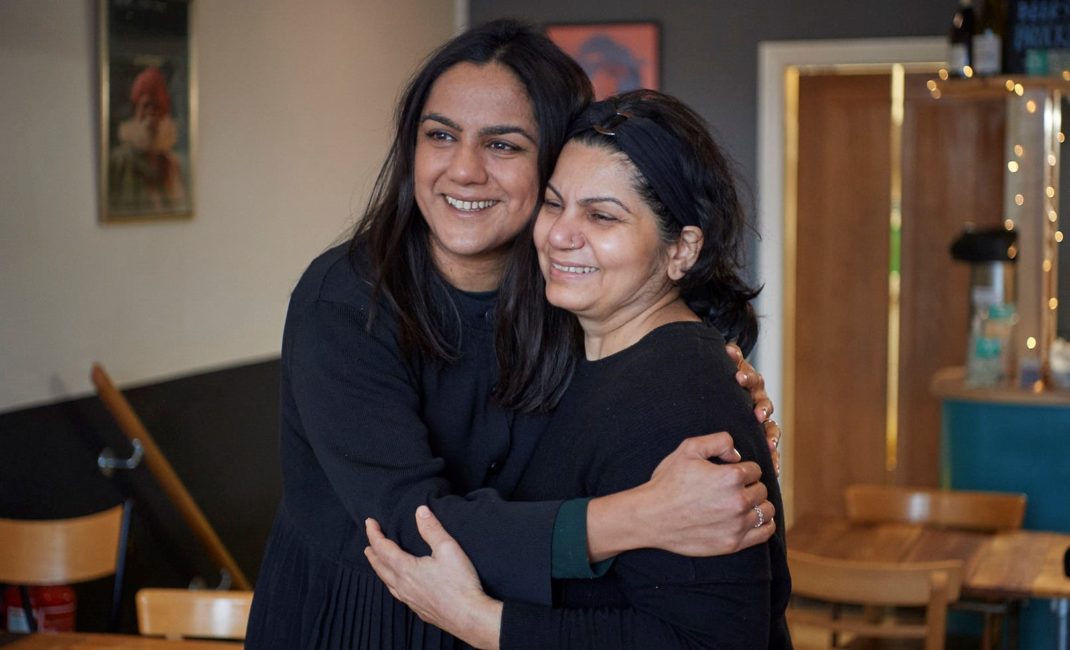
Saima and her mum
There are multiple factors at play here. First there is immigrant shame. Ethnic minorities are conditioned to put our heads down and work hard, we don’t discuss our failures openly, we are merely trying to fit in. That’s the truth for me as a second generation Pakistani as those “head-down, work-hard” values have been deeply instilled in me from a young age.
As a result of this BAME people are not visiting their doctors or discussing possible symptoms amongst their families and peers.
I found that when I turned to the internet and its growing online cancer community to find stories like mine, there really weren’t many ethnic minorities giving their accounts of living with cancer.
Read more: Yes, the fight for Anti-HIV drugs is a fight against discrimination
This left me feeling isolated and alone as the storytelling was predominantly from white women sharing their breast cancer experiences.
My need was for association and recognition of the difficulties I personally faced on top of a life-changing illness.
I have spoken to the top cancer charities and organisations in the UK and asked the question where are the “brown faces”? The feedback is the same: people are “scared” and “ashamed” to come out.
So when it comes to media campaigns you see diversity in faces like a tick-box headcount but there is a distinct lack of storytelling which before my own diagnosis led me to believe that “brown people” didn’t get cancer.

There are also cultural stigmas around illness – that it is possibly “god’s will.” I have even heard personally that my illness is down to “nazar” (black magic).
This then leaves individuals with a lack of ownership or a supportive health plan to recover, prevent and cure potentially treatable illnesses.
Then there is a genuine language and culture barrier as 28% of people do not even understand what their diagnosis means in the UK. How do we cater to those people and make sure they have the right materials and literature, and can make calm, educated decisions about their future health?
As the proud, supposedly multi-cultural society we are in the UK, why is this not reflected in our healthcare system and communities? The message is simple: ethnic minorities need to have better education and opportunities to integrate. The young people need to speak with their elders and health practitioners need to flag up when patients aren’t understanding or being understood so that ethnic minorities stop dying and suffering unnecessarily from potentially treatable and curable conditions.
Follow Saima’s journey via her Curry and Cancer blog.
Saima is an ambassador of Trekstock, a charity working to get young people in their 20s and 30s moving again, when cancer puts their lives on hold.
Editor’s note: Saima died peacefully in late June 2020, surrounded by her loved ones. A tribute from her family commended the lasting impact Saima had on everyone she met. Our thoughts are with Saima’s loved ones.